Risk Factors for ACL Injury

HOW TO KNOW IF YOU ARE AT INCREASED RISK FOR AN ACL INJURY
As we previously described in the blog ACL Injury in Sport, ACL injuries are an EPIDEMIC! Step one of tackling any epidemic is to look at the risk factors. In regards to ACL injury, there are non-modifiable risk factors (things we cannot change) and modifiable risk factors (things we can change). Did you know that an athletes risk of initial ACL injury is 1 in 60 to 1 in 100! The risk of re-injury is 1 in 4! This requires a paradigm shift in order to alter the risk factors before injury.
NON-MODIFIABLE RISK FACTORS
Demographics/ History:
- Gender ➔ Female ➔ 4-6x higher incidence of non-contact ACL injury than males during adolescence
- Age ➔ Females 12-20 years old and Males 14-16 years old
- Prior ACL injury ➔ up to 1 in 4 will tear the same or opposite side
Anatomical/ Genetic Factors:
- Intercondylar Notch / Size of the ACL ➔ the ACL ligament and notch are smaller in females
- A-shaped Notch ➔ indicating a narrower apex ➔ 2.3x greater risk of ACL injury
- Posterior Tibial Slope ➔ Is greater in females ➔ rotational instability of the knee
- Ligamentous Laxity ➔ Females have more genetic ligamentous laxity than men
- Family History of ACL Tear ➔ specific mutations may increase risk for tendon and ACL injury
External Factors
 1. Playing surface ➔ artificial turf ➔ there is an increased incidence of ACL injury. Decreased risk of injury associated with soccer players who play on natural grass with round cleats.
1. Playing surface ➔ artificial turf ➔ there is an increased incidence of ACL injury. Decreased risk of injury associated with soccer players who play on natural grass with round cleats.
2. Footwear ➔ Risk of injury (highest to lowest): Bladed Studded → Soft Ground → Turf → Round studded.
3. Sport ➔ Depending on what sport you play you may be at greater risk for ACL injury.
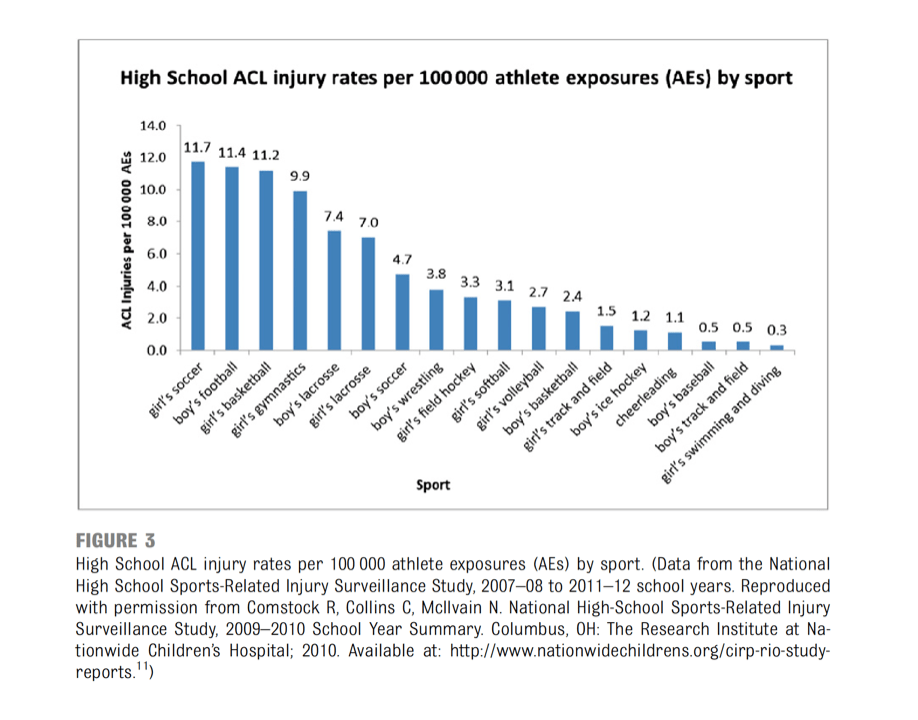
Thank you to Dr. Comstock, Dr. Collins and Natalie Henke (MckIlvain) who provided written permission to use their chart for this blog.
The Big 4: The Major Risk Factors We Can Control To Prevent ACL Injury
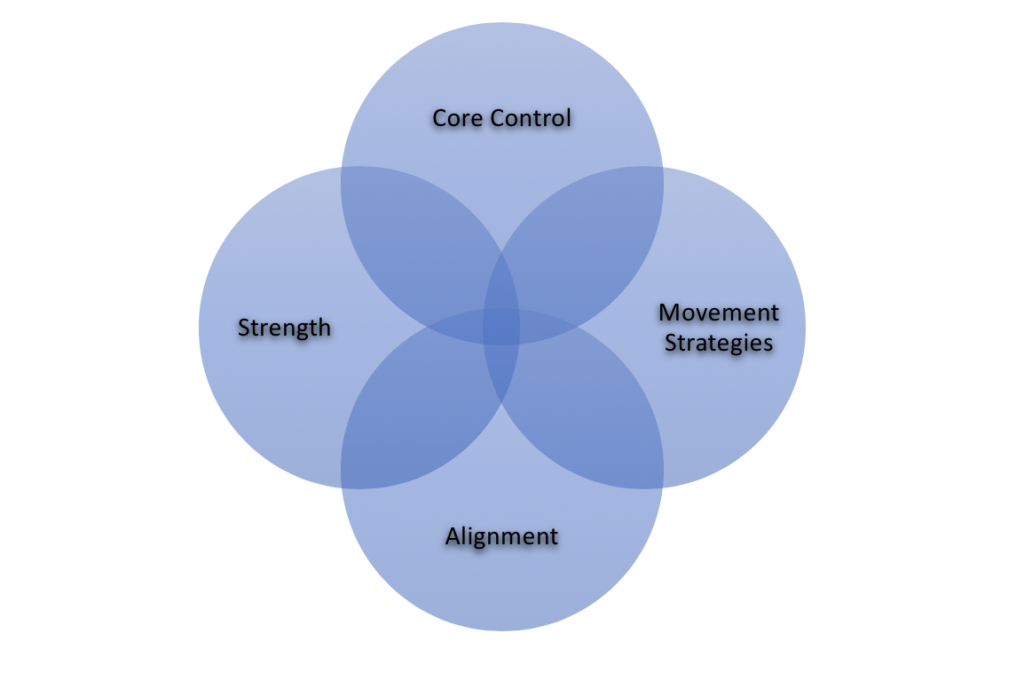
CORE CONTROL
Your core is the structural foundation from which all other movement takes place from. It is made up of your abdominal, pelvic, and back muscles and is responsible for ½ of your entire body mass. A lack of core control contributes to higher risk of ACL injury.
STRENGTH
The powerhouse muscles along your backside from your head all the way down to your feet such as your gluteals and hamstrings are massive muscle groups that aid in creating proper movement patterns and attenuating forces exerted through the body during sport. Proper intervention can help to reduce asymmetries in muscular recruitment and enhance strength from side to side to promote symmetry and enhance performance. Inadequate strength contributes to higher risk of ACL injury.
MOVEMENT STRATEGIES
Females more than males utilize a quad dominant strategy, which means that they land with decreased knee flexion. Landing with decreased knee flexion underutilizes the hamstrings, which are necessary in order to stabilize the ACL. Therefore, quad dominance contributes to higher risk of ACL injury.
ALIGNMENT
Proper foot alignment is important to stabilize the body and help absorb shock during landing. Orthotic intervention plays a vital role in foot alignment and function. A lack of proper foot alignment contributes to higher risk of ACL injury.

Optimal alignment

Abnormal alignment with excessive knee valgus
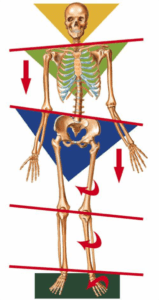
Photo credit: Redcord America
A Forwardly Rotated Pelvis (aka Anterior Pelvic Tilt) creates a functional disadvantage for the core and hamstrings and will facilitate quadriceps dominance. Therefore, a lack of proper pelvic alignment contributes to higher risk of ACL injury.
Summary
In conclusion, core control, strength, movement strategies and alignment are all interconnected, which means it only takes one weak link to create a domino effect among these 4 modifiable variables. We owe it to these athletes to shift the mindset from “reactive” to “proactive” by addressing these modifiable risk factors to help prevent ACL injury.
Stay tuned for the next blog in this series where we talk about ACL injury prevention programs. To learn more about ACL injuries in sport, check out the first blog in this series called “ACL Injury in Sport “.
About The Author
Stephanie Ballis, SPT, has a personal interest in athletics, orthopedic injuries, and the psychological components of recovery. She is a strong proponent of preventative medicine, helping to upstage the ACL prevention research conducted at One on One Physical Therapy in Atlanta, GA. Currently, Stephanie is a physical therapy student in Emory University’s Doctor of Physical Therapy Program. Prior to her matriculation at Emory, she worked in business and sales after graduating cum laude from the University of Denver with a degree in Business Administration and minor in Psychology. Stephanie chose a career in Physical Therapy because she felt that it was the one field that targeted mental and physical well-being simultaneously.
Sources
- Bayer, S., Meredith, S. J., Wilson, K., et al. (2020). Knee Morphological Risk Factors for Anterior Cruciate Ligament Injury. The Journal of Bone and Joint Surgery, 102(8), 703–718. doi: 10.2106/jbjs.19.00535.
- Hewett, T. E., Myer, G. D., Ford, K. R., Paterno, M. V., & Quatman, C. E. (2016). Mechanisms, prediction, and prevention of ACL injuries: Cut risk with three sharpened and validated tools. Journal of Orthopaedic Research, 34(11), 1843–1855. doi: 10.1002/jor.23414.
- Labella, C. R., Hennrikus, W., & Hewett, T. E. (2014). Anterior Cruciate Ligament Injuries: Diagnosis, Treatment, and Prevention. Pediatrics, 133(5). doi: 10.1542/peds.2014-0623.
- Mansfield, M.M. & Bucinell, R.B. (2016). Effects of Playing Surface and Shoe Type on ACL Tears in Soccer Players. American Journal of Engineering and Applied Sciences, 9(4): 1150-1157. doi: 103844/ajeassp.2016.1150.1157.
- Pfeifer, C. E., Beattie, P. F., Sacko, R. S., & Hand, A. (2018). Risk Factors Associated With Non-Contact Anterior Cruciate Ligament Injury: A Systematic Review. International Journal of Sports Physical Therapy, 13(4), 575–587. doi: 10.26603/ijspt20180575.
- Sklar, Joseph MD, PhD (2020, April 18). Orthopedic surgeon. (S. Ballis, Interviewer).